Tight, painful or dimpled scarring

Our private Tight, painful or dimpled scarring services are provided at the Royal Free Hospital, Hampstead.
To find out more about our hospitals click here:
Scars which are tight or painful may restrict your ability to use your residual limb to move a prosthesis. They may be tight if they were placed in a sub-optimal position. Equally they may become tight because it is a fundamental property of scar tissue that it tends to contract over time. If the scar does contract, it may result in dimpling of the overlying skin. This is unsightly and may also lead to issues with hygiene since it is difficult to clean out skin debris from the crevices that form. Scars may also become painful – and this pain is quite separate from neuroma-related pain or phantom limb pain.
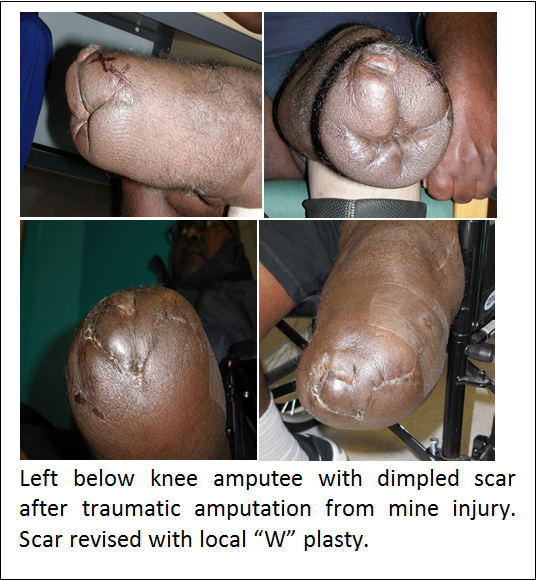
Procedure
Surgery may be used to move your scars away from areas where they can chafe and rub in your socket. To achieve this, it may be necessary to lengthen your scars with Z-plasty releases or by moving the tissues around on your residual limb using local flaps. Dimpled scars benefit from release of the skin from the deeper tissues which are causing the scars to contract. However, over time (years), the dimpling may recur.
Scars may become particularly painful and sensitive if they are hypertrophic. Scars are described as hypertrophic if they are red and raised. This type of scar responds well to regular injections of steroids directly into the scar. The injections are administered in clinic every 6 weeks until the scar responds.
Pre and Post-op Management
Anaesthetic: Patients undergoing scar revision surgery usually require a regional block (e.g. axillary or spinal anaesthetic) or a general anaesthetic. You can discuss your specific requirements with our anaesthetists before surgery.
Length of stay: Depending on the amount of tissue that needs to be excised, you may be able to have your surgery as a daycase procedure or have an overnight stay before going home.
Pain control: Pain levels after surgery vary from one individual to the next. In general, pain levels after this type of surgery are usually relatively low and can be managed with simple opiates (e.g. codeine or tramadol) taken orally for a few days. Discuss your specific requirements with your anaesthetist before discharge.
Wound care: Wound care after this type of surgery is usually simple. You can shower immediately but not soak your wounds in a bath for 2 -3 weeks. Running water is fine. If you do shower, your dressings will get wet and will probably come off. Do not worry. We will supply you with adhesive dressings to replace them. Pat your wound dry with clean tissue paper and leave your wound exposed to the air for 15-30 minutes. Then apply a new adhesive dressing.
Rehabilitation: Although you do not need any specific rehabilitation exercises after this type of soft-tissue surgery, the shape of your residual limb will of course change, both temporarily and in the long-term. It is likely that you will be unable to use your standard socket immediately after surgery both to avoid problems with your new wound and because your residual limb will be swollen. Once your wounds have healed and any swelling has settled, you will need to have a new socket fitted to your residual limb.
Get in touch
