Bowel cancer is the third most common cancer and second cause of cancer related death in the UK. To date there is no direct cause of bowel cancer and although a poor diet and lifestyle are contributory, there are also genetic factors that can be passed down generations.
While it is more likely to come as we grow beyond our 60s, we are now seeing those in their 30s and 40s presenting with bowel cancer. It is a slow growing cancer so if diagnosed early can lead to a complete cure. The main symptoms of bowel cancer are blood in the poo, a change in bowel opening frequency, either more loose or more constipated or an alteration between. Some patients may also present with lower tummy pain.

If one were to have these symptoms, they should see their doctor and be referred for a colonoscopy, which is a camera inserted through the back passage to investigate their symptoms. The majority of patients undergoing this procedure will not have bowel cancer but other benign conditions can be diagnosed and pre-cancerous growths (polyps) could be removed. There are a group of patients that may not be appropriate for a colonoscopy and for those, a scan can be arranged.
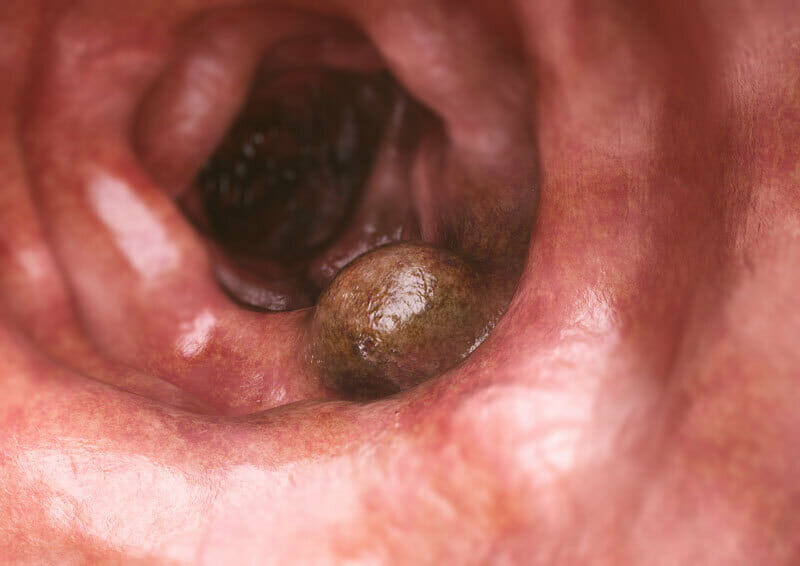
If bowel cancer is diagnosed, other scans are arranged to determine whether the cancer has spread or not and the patient is then referred to a colorectal surgeon who will discuss their case in a multidisciplinary meeting (MDT) to determine the best course of action for treatment. This treatment may involve surgery, chemotherapy or radiotherapy.
Colorectal cancer surgery
We perform cancer surgery in a minimally invasive way using laparoscopic (keyhole) or robotic methods to ensure small incisions, a faster recovery and reduced risks of developing hernias. Once treated, bowel cancer is then monitored by the colorectal surgeon for the next five years to ensure it does not return. This monitoring phase is usually undertaken with regular scans, blood tests and colonoscopies.
About the author: Mr Ibnauf Suliman is a Consultant Colorectal and General Surgeon with a specialist interest in minimally invasive surgery. His practice includes colorectal cancer, inflammatory bowel disease, and proctology as well as elective and emergency general surgery. His colorectal fellowships in laparoscopic, robotic, pelvic floor, and exenterative surgery have brought this experience into his clinical practice. He is an examiner at UCL Medical School and enjoys teaching junior surgeons. To know more about Mr Suliman, please click here.
